Breathe Easier in Raleigh Nights Sleep apnea is a breathing problem that happens while you sleep. Your airway partly or fully closes, so you stop and start breathing again and again. Many people in Raleigh have busy, high-stress days, late nights, and early mornings. It is easy to blame poor sleep on work, kids, or…
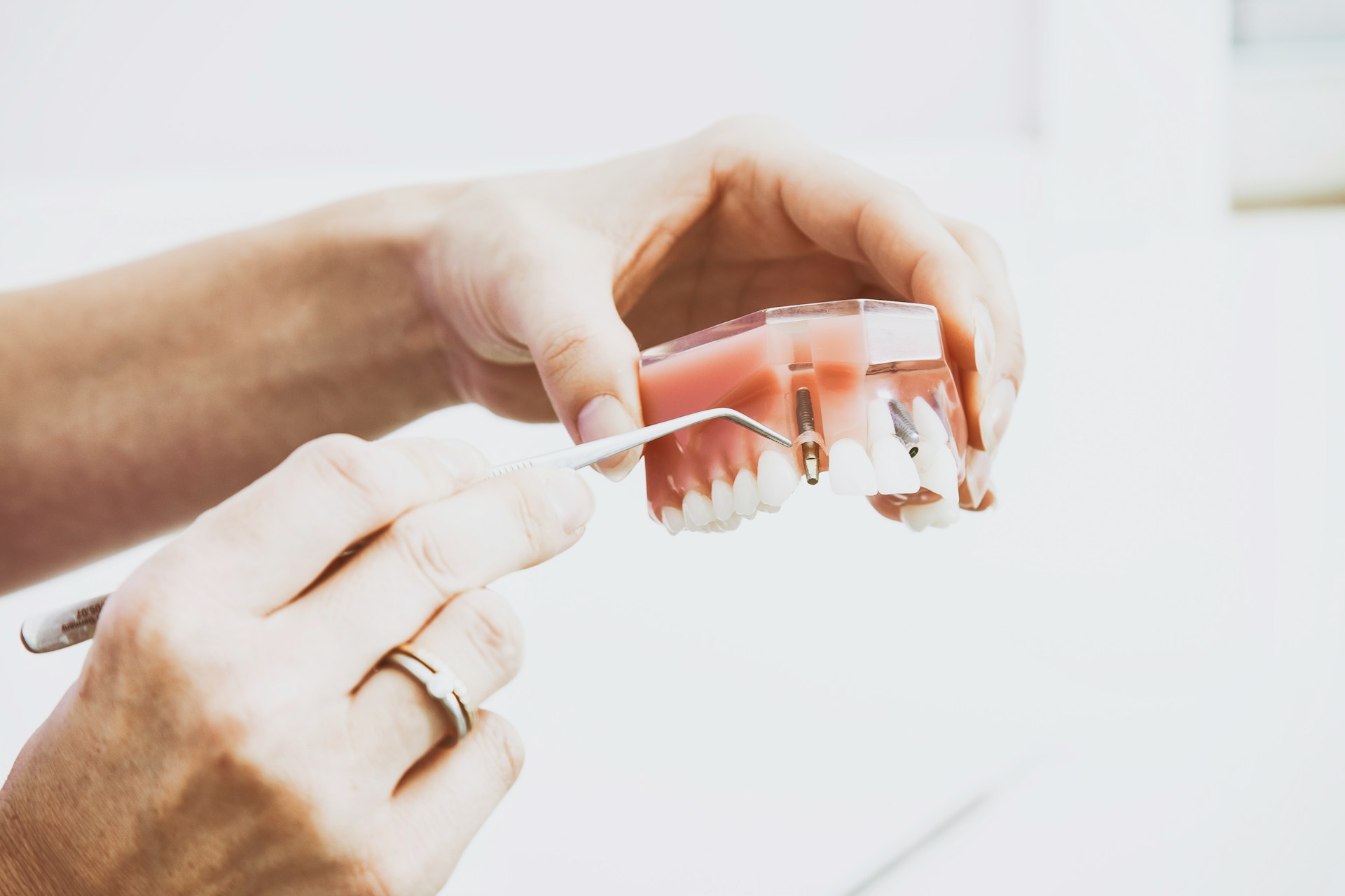
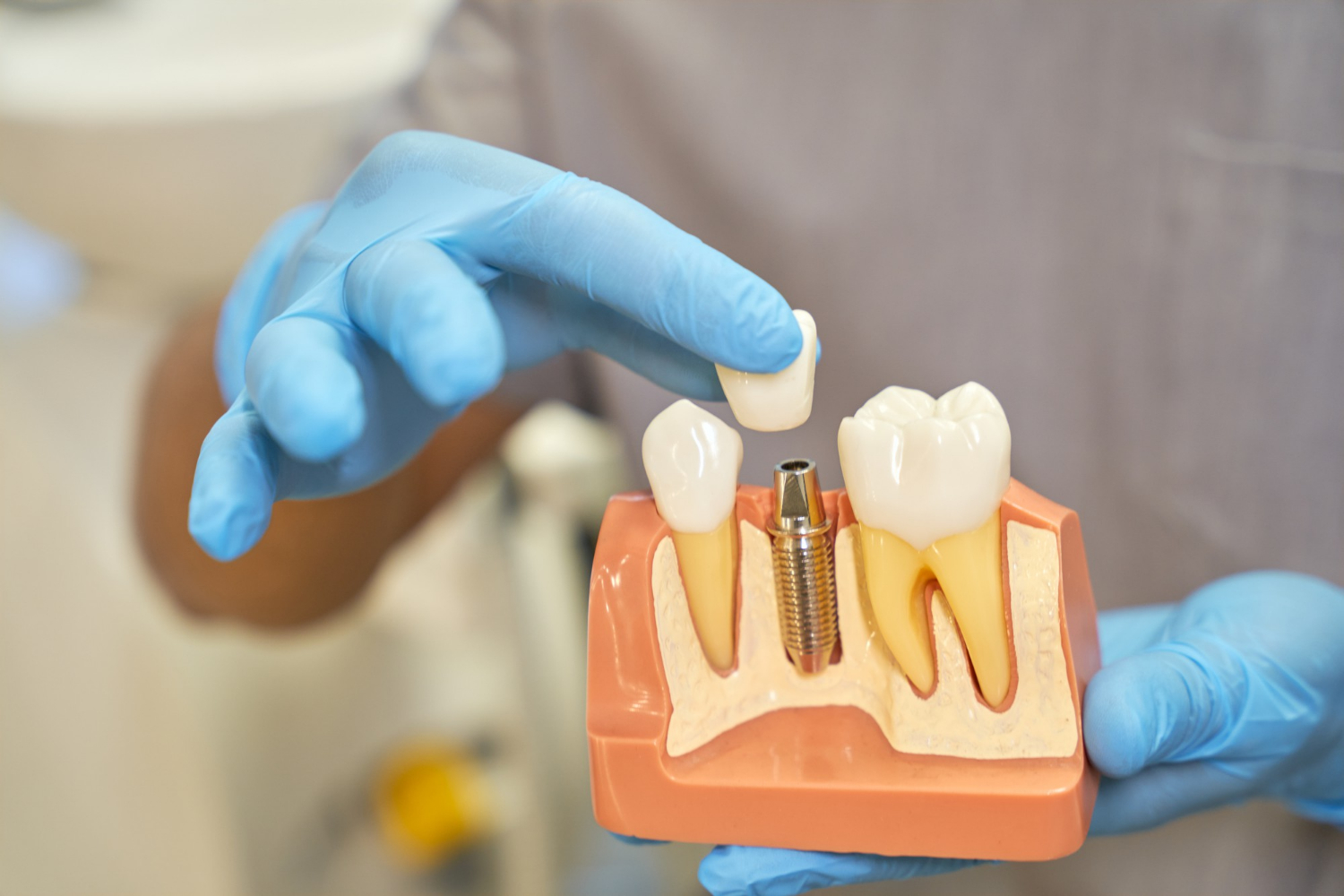
Protect Your Dental Implants Before Summer Starts Dental implants are a big investment in your smile, your comfort, and your confidence. Like anything you care about, they need a little attention to stay in great shape, especially before life gets busy with trips, sports, and outdoor plans. Spring and early summer are a smart time…
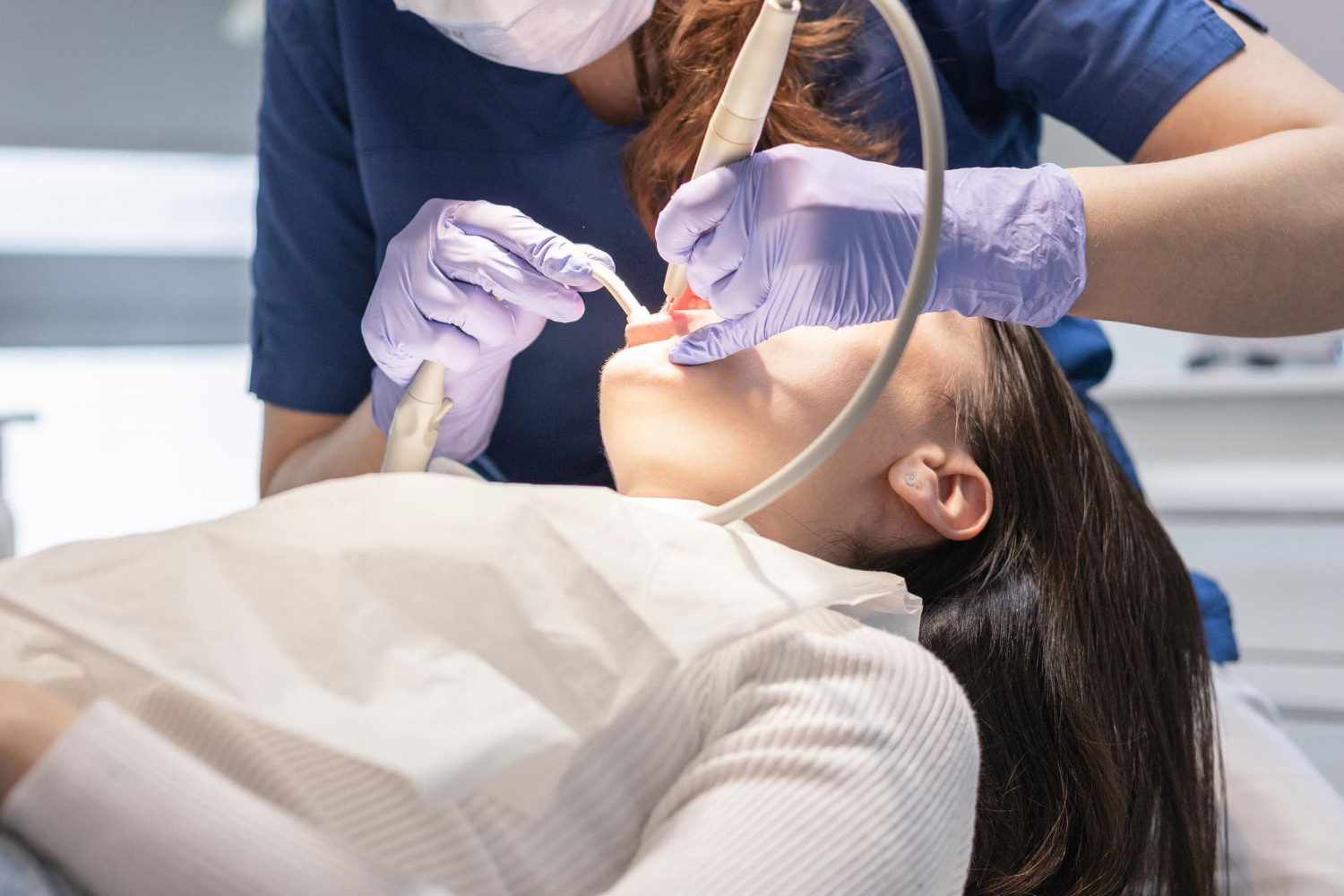
Confident Dental Visits When Your Health Is Complicated Dental visits can feel heavy when you already have a full plate of medical issues. Many people with heart disease, diabetes, cancer treatment, autoimmune conditions, or weakened immune systems delay care because they worry about pain, fatigue, infection risk, or how their medications might mix with numbing…
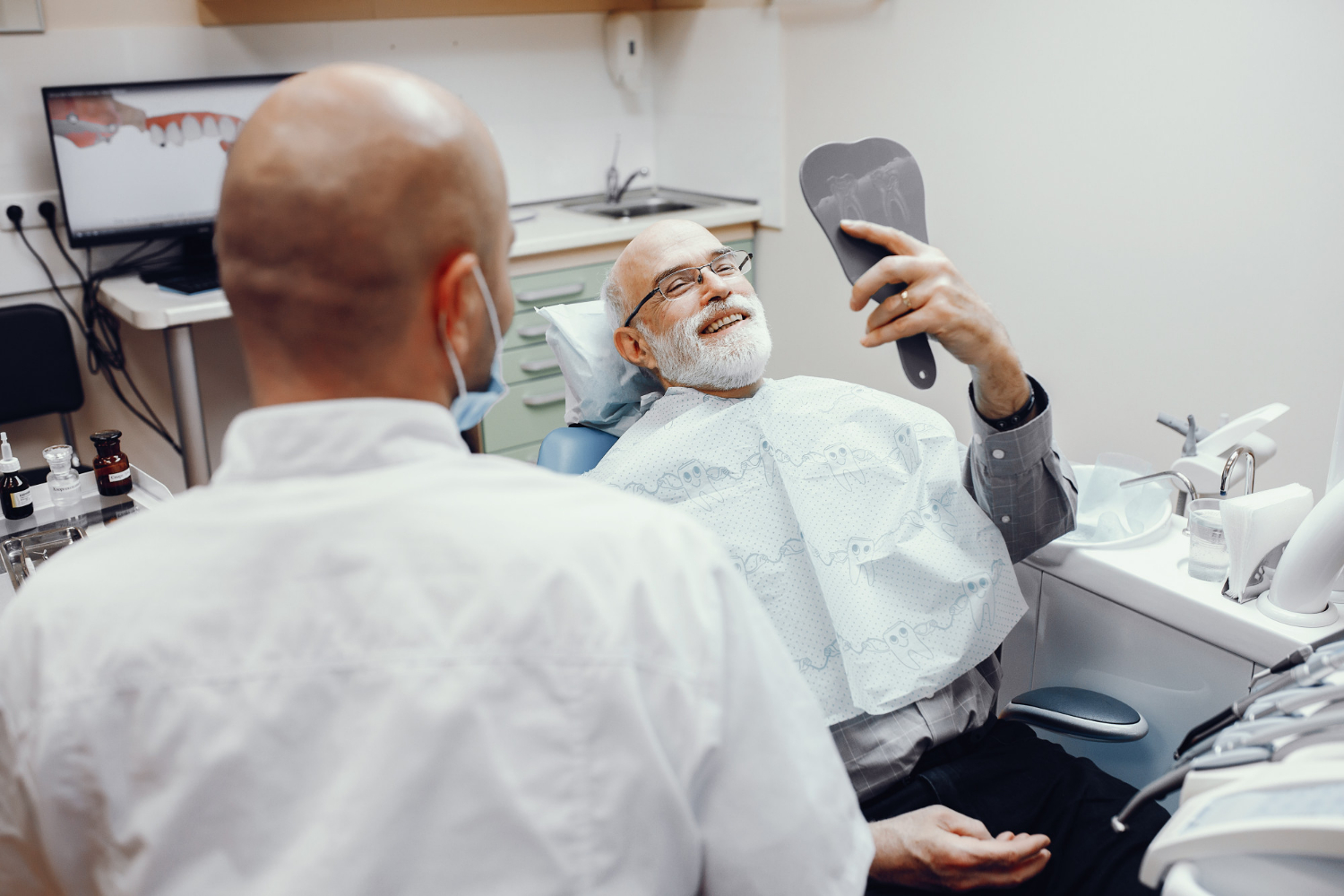
Enjoy More Freedom and Confidence as You Age Missing teeth or loose dentures can make everyday life harder than it needs to be. Simple things like sharing a meal, singing at church, or smiling for a family photo can start to feel stressful. Many seniors around Raleigh reach a point where they are tired of…
Protect Your Spring Smile Investment with Healthy Gums Dental implants are a smart way to replace missing teeth, especially when you want to feel confident in photos, at parties, and at get-togethers. Spring often feels like the perfect time to move forward, since many people are getting ready for weddings, graduations, vacations, and more social…
Recognizing Dental Emergencies Before Visiting a Raleigh ER When a tooth suddenly hurts or a front tooth gets chipped, it can be scary and stressful. In that moment, it is hard to know if you should head straight to the ER or call a dentist first. Knowing the difference can save you time, worry, and…
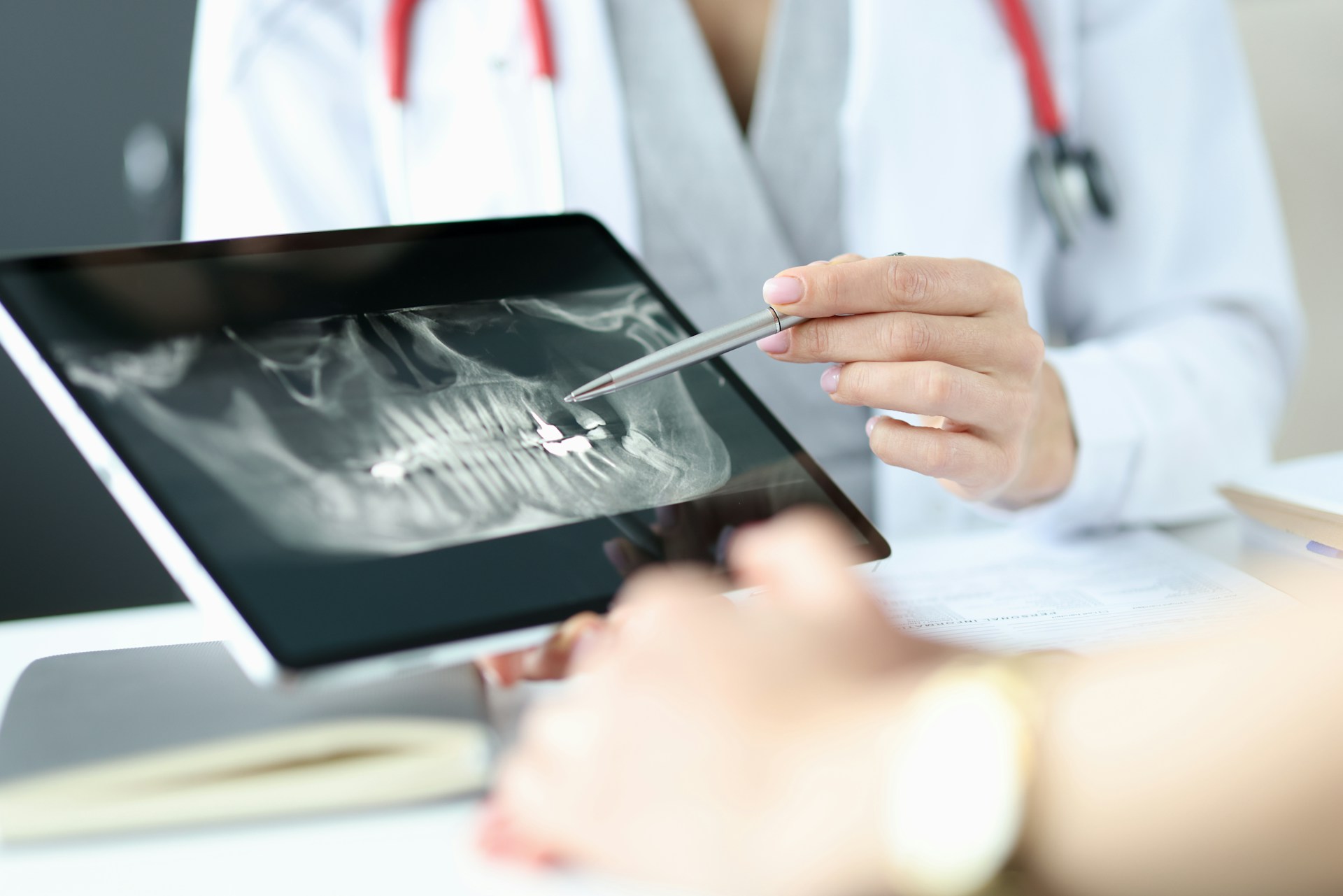
How Your Dentist May Be the First to Spot Sleep Apnea Feeling wiped out before the day even starts, hitting snooze again and again, or blaming that heavy morning fog on allergies or the time change is common. Many people chalk it up to stress or getting older and push through it. But sometimes that…
Catch Dental Implant Problems Before Summer Starts Dental implants can be a great way to replace missing teeth. They look natural, feel secure, and let you chew and smile with confidence. Many adults in Raleigh choose them because they want something that stays in place and does not come in and out like a denture.…
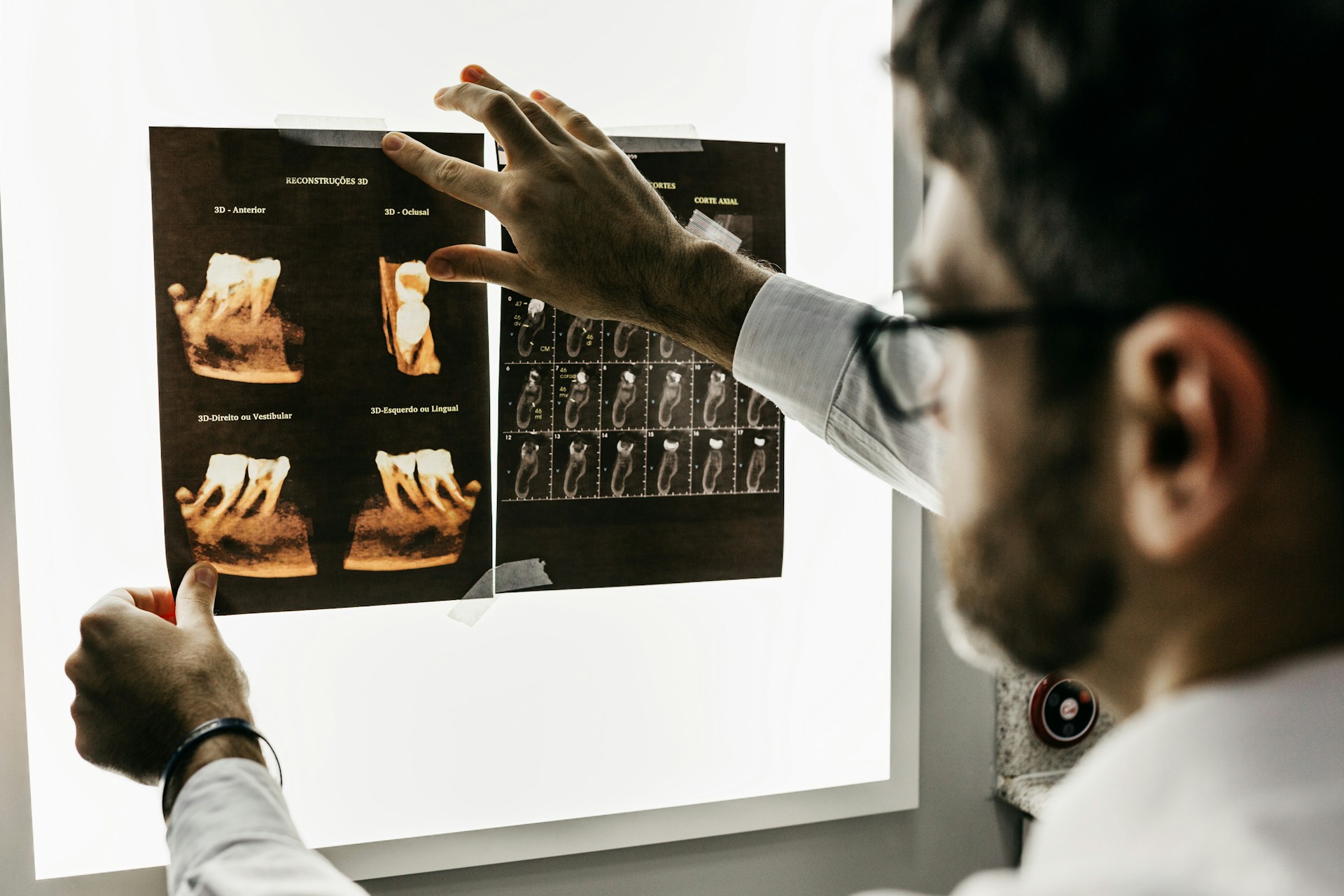
Recognizing Dental Implant Problems Early with a Raleigh Dentist Healthy dental implants should feel almost as natural as your own teeth. When something starts to feel off, even in a small way, your mouth is trying to tell you something. Catching those early changes can help protect your smile, your comfort, and the investment you…
Protect Your Implants by Catching Gum Disease Early Healthy gums are the foundation of every strong smile, especially if you have dental implants or crowns. When the gums start to break down, it can put those restorations at risk long before you feel pain. Gum disease often starts quietly, so by the time it hurts,…